
A 90-day delay in provider enrollment and credentialing for a single physician can put hundreds of thousands, and in some specialties, over $1 million, in revenue at risk.
When enrollment timelines drag, practices can’t bill payers, claims are denied, and cash flow slows. Yet many organizations still treat provider enrollment and credentialing as an administrative checklist instead of a core revenue protection strategy.
For physician practices, behavioral health groups, RHCs, FQHCs, and hospitals, inefficient credentialing creates avoidable financial strain, especially during onboarding of new providers.
At Legacy Consulting Services, we help healthcare organizations streamline enrollment processes so providers can bill sooner, reduce denials, and protect revenue from day one.
Let’s break this down.
What Is Provider Enrollment in Healthcare?

Provider enrollment is the formal process of registering a healthcare provider with insurance payors so the organization can submit claims and receive reimbursement for services rendered.
Provider enrollment typically includes submitting applications, verifying licensure and credentials, establishing effective dates, and linking providers to the correct Tax Identification Number (TIN) and practice location.
Without approved provider enrollment, claims will deny, reimbursement will be delayed, or payment may be permanently forfeited.
Which Payors Require Provider Enrollment?
Most payors require provider enrollment before claims can be submitted and paid, including:
- Medicare
- Medicaid (state-specific programs)
- Commercial insurance carriers
- Managed care organizations
- Marketplace exchange plans
- CAQH (Council for Affordable Quality Healthcare)
- State-specific and regional payors
Each payor maintains its own application process, documentation requirements, and approval timelines. Enrollment must often be completed at both the individual provider level and the group or facility level.
Failing to enroll correctly with even one payor can result in denied claims, retroactive billing limitations, and significant revenue disruption.
What Is Medical Credentialing?

Medical credentialing is the formal verification process used by payors to confirm that a healthcare provider meets professional, legal, and regulatory standards to deliver care.
During medical credentialing, payors review and validate a provider’s:
- Education and training
- Active state licensure
- Board certification status
- Work history
- DEA registration (if applicable)
- Malpractice insurance coverage
- Sanctions or exclusion history
Unlike provider enrollment, which registers a provider for billing purposes, medical credentialing verifies qualifications and determines whether a provider meets participation standards.
Payors will not release reimbursement until credentialing is fully reviewed and approved — even if services have already been rendered.
What Does the Credentialing Verification Process Include?
The credentialing verification process typically includes:
- Primary source verification of licensure and board certification
- Review of the National Practitioner Data Bank (NPDB)
- OIG and exclusion list screening
- Confirmation of malpractice coverage and claims history
- Validation of work history and any gaps in employment
- CAQH profile review and attestation
Each payor conducts its own review and may request additional documentation or clarification during the process.
Incomplete applications, outdated CAQH profiles, discrepancies in work history, or missing documentation are common causes of delays. These issues can extend approval timelines by weeks, or even months, directly impacting reimbursement.
Why Credentialing Delays Cause Revenue Loss

Credentialing delays create immediate and measurable revenue disruption.
Here’s what typically happens:
- A new provider begins seeing patients.
- Provider enrollment and credentialing are still “in process.”
- Claims are submitted under the assumption approval is pending.
- Claims deny due to non-participation or inactive status.
- Appeals are submitted, often with limited success.
- Reimbursement is delayed, or permanently written off.
Many practices assume retroactive billing will resolve the issue. In reality, retroactive approvals are limited, inconsistent, and often do not cover the full date of service range.
Even short enrollment gaps can create significant cash flow strain.
The Real Cost of Enrollment Delays by Specialty
The financial impact of credentialing delays varies by specialty, patient volume, and payer mix.
High-volume or procedure-based specialties, such as orthopedics, cardiology, gastroenterology, and behavioral health , can experience substantial daily revenue disruption when enrollment is not finalized.
For hospital-employed providers and group practices, even one delayed approval can affect downstream services, facility fees, and ancillary billing.
Credentialing is not simply an administrative timeline , it is a revenue activation trigger.
How Much Revenue Does a Specialist Lose Per Day Without Credentialing?
Revenue loss depends on average daily charges and reimbursement rates, but for many specialists:
- Daily billable revenue can range from $5,000 to $25,000+
- A 60–90 day delay can translate into hundreds of thousands of dollars in delayed or unrecoverable reimbursement
While some claims may be recoverable, many practices face filing limits, retroactive participation restrictions, or partial payment reductions.
The longer provider enrollment and credentialing remain incomplete, the greater the financial exposure.
Revenue Loss by Specialty – Real Numbers
The financial impact of provider enrollment and credentialing delays is real. A single provider generating $1,200 per day across 20 days a month represents $24,000 in potential revenue. A 90-day delay puts $72,000 at risk, and a five-provider group could face $360,000 or more, before considering cash flow strain, staff rework, patient frustration, or contracting issues.
Revenue impact varies by specialty, payer mix, and service type, but even conservative estimates show how quickly delayed credentialing can create significant financial exposure.
Here are realistic national averages:
General Surgeon
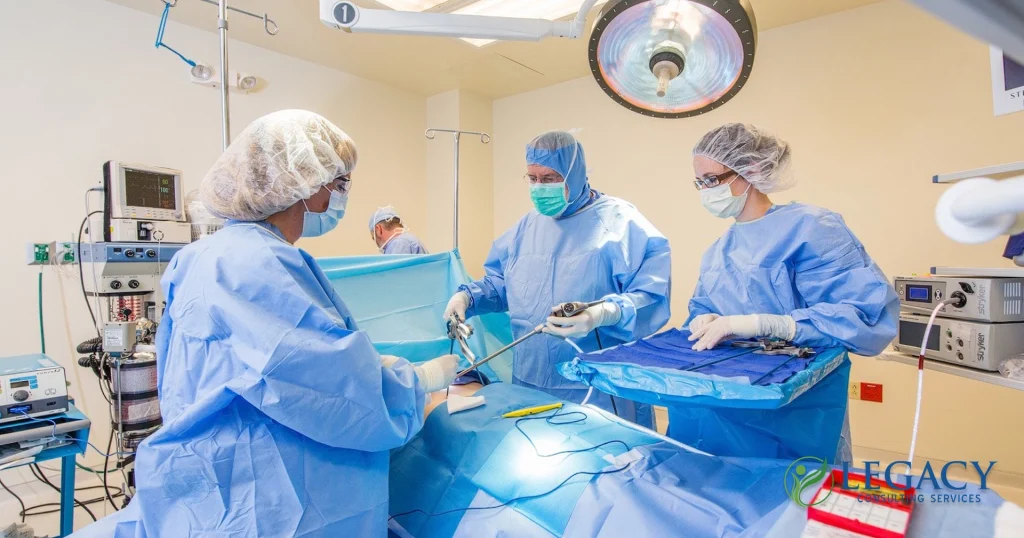
Typical Production:
- 3–6 surgical cases per day
- $3,000–$7,000 gross revenue per case (blended average)
- Plus office consults
Estimated Daily Gross Revenue:
$15,000 – $30,000 per day
Even conservatively:
- $18,000/day x 60-day delay = $1,080,000 at risk
Not all of that is net income, but that is revenue the hospital or practice cannot bill if credentialing is incomplete.
Cardiologist (Non-Invasive)

Typical Production:
- 20–30 patients/day
- Echo, stress tests, EKG interpretations
- Some procedure billing
Estimated Daily Gross Revenue:
$8,000 – $15,000 per day
If they also read imaging or supervise tests:
$15,000 – $20,000/day
A 90-day delay:
- $12,000/day average x 90 days = $1,080,000 at risk
Interventional Cardiologist
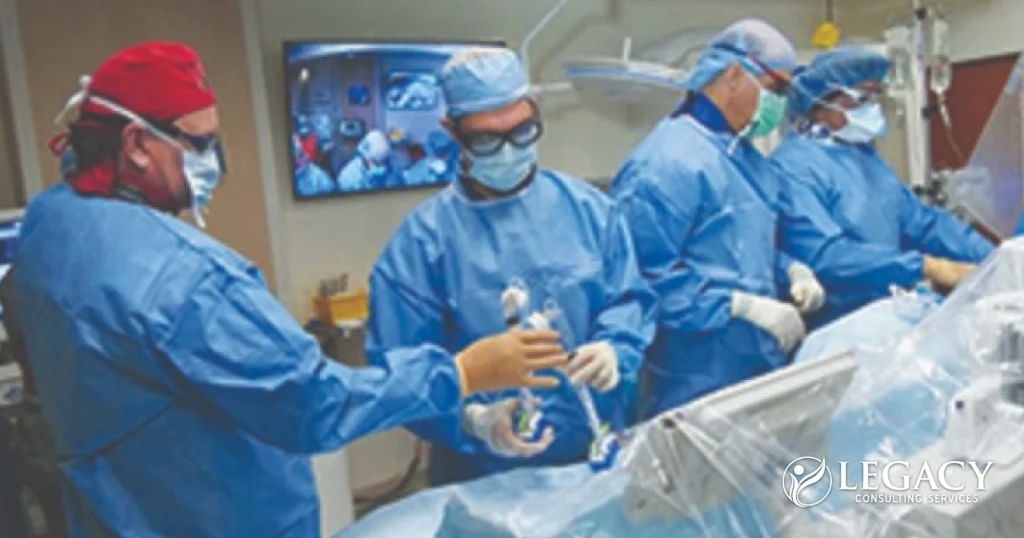
Typical Production:
- Cath lab procedures
- Angioplasty/stents
- Inpatient consults
Estimated Daily Gross Revenue:
$20,000 – $50,000 per day
A 60-day delay:
- $30,000/day x 60 days = $1.8 million exposure
Orthopedic Surgeon

Typical Production:
- Joint replacements
- Arthroscopy
- Fracture repair
- Clinic visits
Estimated Daily Gross Revenue:
$20,000 – $60,000 per day
Even if you use a conservative blended rate:
$25,000/day
90-day delay:
- $25,000 x 90 = $2.25 million at risk
Neurosurgeon
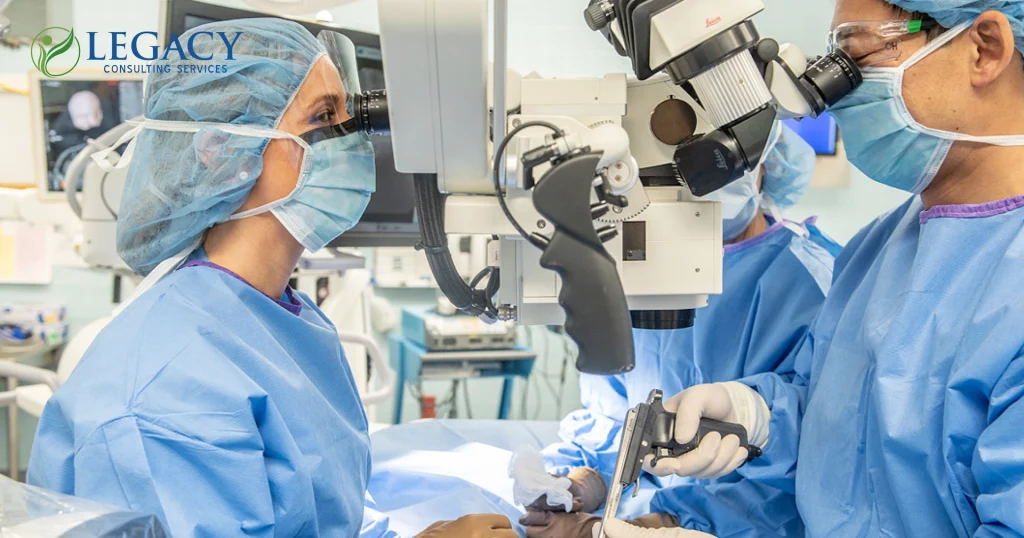
Typical Production:
- Spine cases
- Brain surgery
- Complex inpatient procedures
Estimated Daily Gross Revenue:
$30,000 – $100,000 per day
This is why hospitals panic when neurosurgeons are not enrolled correctly.
What This Means for Hospitals & Groups
For primary care:
- 60-day delay might cost $100,000–$200,000
For specialists:
- 60–90 days can cost $1–3+ million per provider
And here’s the key:
Most hospitals don’t even realize the exposure until cash flow drops.
Top Reasons Claims Deny Due to Credentialing Issues
- Incorrect effective dates
- Missing CAQH attestations
- TIN/NPI mismatches
- Group vs individual enrollment errors
- Location-specific enrollment gaps
- State Medicaid revalidation failures
- Expired licenses or malpractice documentation
These are preventable.
How to Avoid Credentialing Denials: 5 Best Practices
Preventing credentialing denials requires proactive planning, consistent monitoring, and alignment between enrollment, billing, and contracting. The following best practices help protect revenue and minimize disruption.
Start Provider Enrollment 120–180 Days Before Start Date
Provider enrollment and credentialing should begin well before a new hire’s first day. Most commercial payors require 60–120 days for approval, while Medicare and Medicaid can take longer depending on the state. Early submission reduces the risk of revenue gaps when the provider begins seeing patients.
Maintain Active CAQH Management
An incomplete or outdated CAQH profile is one of the most common causes of enrollment delays. Quarterly attestations, updated malpractice documentation, and accurate work history are essential to prevent processing setbacks.
Track Payor Effective Dates
Approval alone is not enough. Billing must align precisely with the payor’s assigned effective date. Submitting claims outside the approved participation window will result in denials, even if credentialing is technically complete.
Align Credentialing with Payor Contracting
Being credentialed does not automatically mean the provider is contracted at optimal reimbursement rates. Enrollment and contracting should be coordinated to ensure appropriate fee schedules are in place before services are billed.
Conduct Annual Enrollment Audits
Provider enrollment is not a one-time task. Revalidations, PECOS updates, Medicaid recredentialing cycles, ownership changes, and TIN updates must be monitored regularly. Annual audits help prevent lapses that can interrupt reimbursement.
Why Retroactive Billing Is Not a Reliable Safety Net
- Some commercial payors do NOT allow retroactive effective dates.
- Medicaid is state-dependent.
- Medicare may allow limited retroactivity.
- Surgical global periods complicate back billing.
If effective dates are wrong? Revenue is written off.
Signs Your Practice Needs a Credentialing Audit
- New providers are seeing patients but revenue is delayed
- Frequent non-par denials
- Retroactive billing appeals are common
- CAQH management is inconsistent
- Medicaid revalidations are missed
- Providers are not loaded under all practice locations
- You suspect reimbursement rates are lower than contracted
How Legacy Consulting Services Accelerates Revenue Through Credentialing
At Legacy Consulting Services, we go beyond transactional credentialing. We take a revenue-first approach, treating provider enrollment and credentialing as a strategic tool — not just paperwork.
We help practices:
- Create provider enrollment timelines and monitor progress
- Audit active payor participation and track effective dates
- Align enrollment with payor contracting to optimize reimbursement
- Prevent write-offs and identify reimbursement gaps
- Accelerate billing start dates
We also integrate credentialing with:
- Revenue cycle management
- Billing integrity audits
- Payor contract negotiations
- Zero balance claim reviews
Because at the core, credentialing is revenue strategy , not administrative overhead.
Strategic Positioning for Legacy Consulting Services
Credentialing is not clerical work. For high-producing specialists, even a two-week delay can represent $200,000–$500,000 in deferred revenue.
By approaching enrollment and credentialing strategically, Legacy helps practices achieve:
- Revenue acceleration
- Cash flow protection
- Risk mitigation
- Contract alignment
- Infrastructure optimization
This is an executive-level strategy, ensuring that provider onboarding drives revenue rather than delays it.
Frequently Asked Questions: Provider Enrollment and Credentialing
Provider enrollment and credentialing timelines, requirements, and payer rules can vary widely. Below are answers to some of the most common questions healthcare organizations ask when navigating the enrollment process.
How long does provider credentialing take?
Typically 60–120 days for commercial carriers and 90–150 days for Medicare or Medicaid, depending on the state.
Can you bill before credentialing is approved?
In most cases, no. Claims will deny unless retroactive approval is granted.
What is the difference between enrollment and credentialing?
Enrollment registers the provider with the payor. Credentialing verifies qualifications. Both must be completed before payment.
Why are my claims denying for non-participation?
The provider may not be fully enrolled, the effective date may be incorrect, or the TIN/NPI combination may not be linked properly.
How can I speed up provider enrollment?
Early submission, complete documentation, CAQH accuracy, and active follow-up significantly reduce delays.
Ready to Evaluate Your Credentialing Process?
Legacy Consulting Services helps practices streamline provider enrollment and credentialing to maximize cash flow and minimize claim denials. Our services include:
- Provider enrollment audits
- Full-service credentialing management
- Payor contracting alignment
- Revenue cycle integration
- Reimbursement optimization strategies
Don’t wait until a new provider starts seeing patients. Schedule a credentialing assessment today and ensure your practice is set up to bill accurately, on time, and at optimal rates.

